Abstract
Importance
Oculomics is the science of analyzing ocular data to identify, diagnose, and manage systemic disease. This article focuses on prescreening, its use with retinal images analyzed by artificial intelligence (AI), to identify ocular or systemic disease or potential disease in asymptomatic individuals. The implementation of prescreening in a coordinated care system, defined as Healthcare From the Eye prescreening, has the potential to improve access, affordability, equity, quality, and safety of health care on a global level. Stakeholders include physicians, payers, policymakers, regulators and representatives from industry, government, and data privacy sectors.
Observations
The combination of AI analysis of ocular data with automated technologies that capture images during routine eye examinations enables prescreening of large populations for chronic disease. Retinal images can be acquired during either a routine eye examination or in settings outside of eye care with readily accessible, safe, quick, and noninvasive retinal imaging devices. The outcome of such an examination can then be digitally communicated across relevant stakeholders in a coordinated fashion to direct a patient to screening and monitoring services. Such an approach offers the opportunity to transform health care delivery and improve early disease detection, improve access to care, enhance equity especially in rural and underserved communities, and reduce costs.
Conclusions and Relevance
With effective implementation and collaboration among key stakeholders, this approach has the potential to contribute to an equitable and effective health care system.
JAMA Ophthalmol. doi:10.1001/jamaophthalmol.2025.0881
Current health care systems are burdened with high costs, limited accessibility, and delayed disease identification. Integration of artificial intelligence (AI) within health care holds promise to mitigate these challenges by improving disease detection and outcomes across diverse socioeconomic groups, potentially reducing costs and increasing access. Given these challenges and recent technological advancements, the broader adoption of AI into health care settings already has begun. The process of extracting systemic health insights by analyzing ocular data, including retinal images with AI, is referred to as oculomics. We define prescreening as a preliminary assessment of disease or potential disease in asymptomatic individuals. Healthcare From the Eye (Topcon Healthcare Inc) prescreening is utilization of retinal images to identify ocular or systemic disease or potential disease in asymptomatic individuals in a coordinated care system that includes eye care professionals (ECPs), primary care professionals (PCPs), and specialty care professionals using secure and responsible technology. It offers the potential for rapid, cost-effective, and accessible prescreening for a wide range of devastating diseases. Such an initiative has the potential to triage asymptomatic patients for screenings where doctors can perform medical tests to check for disease and health conditions, accompanied by follow-up monitoring when applicable. Not only should this have the potential to reduce soaring health care expenditures, but it also might help address chronic disease burdens worldwide by facilitating earlier detection for timely clinical management, leading to better patient outcomes and optimized utilization of health care resources.
To expedite AI integration into health care, various initiatives are under way to establish guidelines, policies and laws for the responsible use of AI, including efforts by the World Health Organization and the US Food and Drug Administration (FDA). Other endeavors aim to develop a code of conduct focusing on AI ethics, equity, and postimplementation. By incorporating perspectives from academia, health care systems, and the health care industry, broad principles and recommendations are considered here.
Why the Eye?
Beyond vision, the eye offers a noninvasive view of microvascular and neurological structures that provide valuable insights into systemic health. Advancements in ophthalmic diagnostic imaging technologies have led to 3-dimensional (3-D) structural optical coherence tomography (OCT) and 3-D vascular OCT angiography, enabling assessment of micron-level changes to disease biomarkers. Such technologies might facilitate early and precise disease management strategies by providing insights into pathological changes at a subcellular level. Peer-reviewed studies have consistently demonstrated a strong correlation between retinal images and the detection of multiple systemic diseases, including, but not limited to, cardiovascular disease (CVD), chronic kidney disease (CKD), and Alzheimer disease.
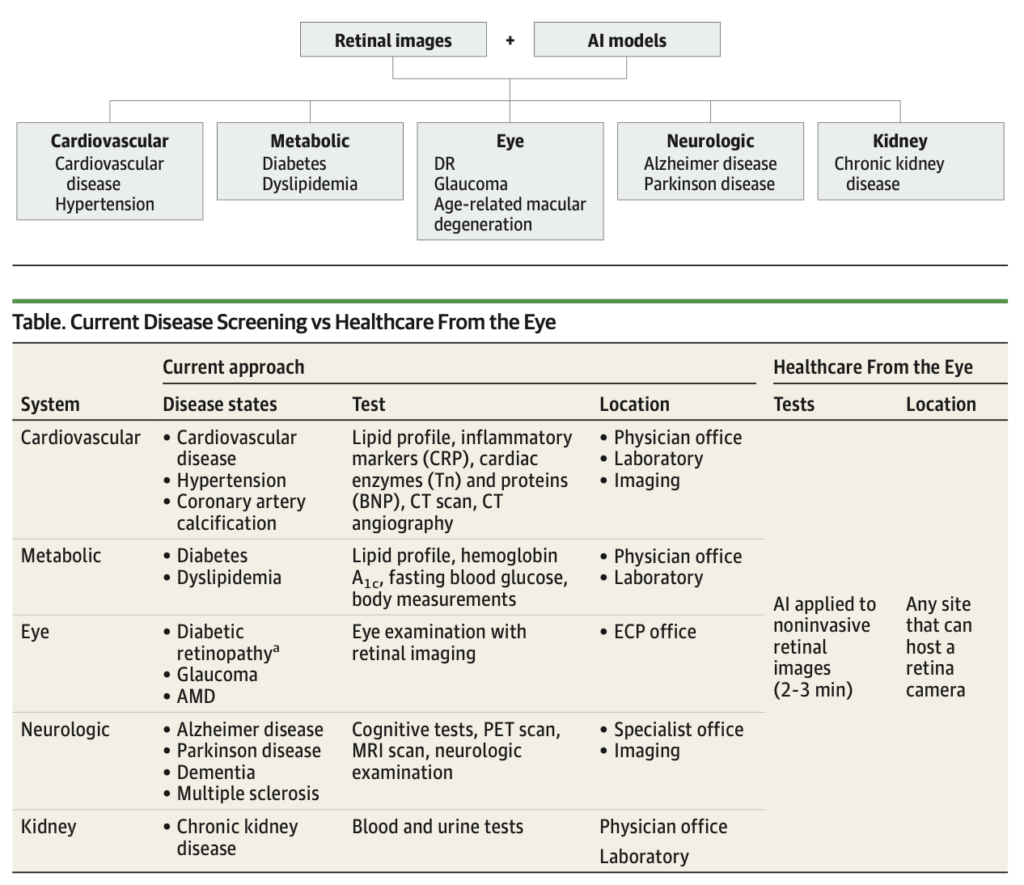
Besides the robust scientific rationale, several operational factors contribute to the feasibility of using the retina for health assessments and prescreenings. First, regular ophthalmic examinations are conducted for both adults and children. Second, automated ophthalmic imaging devices rapidly capture high-resolution retinal images that are safe, noninvasive, and relatively inexpensive compared with other diagnostic methods such as computer tomography scans, ultrasound imaging, electrocardiograms, and blood draws. Moreover, these devices are increasingly being placed in eye care centers and PCP offices. The accessibility of this imaging technology potentially further enhances the feasibility of Healthcare From the Eye prescreening. Third, many vision and medical insurance plans (eg, Medicare Advantage) cover annual eye examinations. Images captured during these examinations could be leveraged for prescreening, particularly for patients with chronic conditions at risk of blindness, including racial and ethnic minority youth with diabetes.
Expanding Healthcare From the Eye prescreening to more than 60,000 ECPs and 270,000 PCPs across the US is a compelling idea for enabling earlier detection of systemic conditions, in addition to ocular conditions.
What is Healthcare From the Eye and Who Benefits?
Healthcare From the Eye prescreening is a proactive approach that applies validated AI-powered applications to high-resolution retinal images in an evidence-based approach to identify a wide range of ocular and systemic conditions. Some PCPs are already capturing retinal images of their patients living with diabetes to screen for referable diabetic retinopathy (DR). A few examples are Stanford University’s and University of California, San Diego’s implementation of a distributed model that integrates eye screening into primary care using AI technology. These initiatives may increase compliance with DR screening and may facilitate effective communication of results to both patients and their PCPs, thereby enhancing patient counseling and closing the loop on the screening process. Additional studies are needed to understand the magnitude of this to patients or their PCPs or both.
With the FDA-cleared fully autonomous AI algorithms that identify referrable and/or treatable DR within minutes while the patient is on site, the adoption of DR screening in PCP settings may increase. Autonomous detection of referrable DR is now possible using portable or handheld cameras within a few minutes, enabling the possibility of health care professionals (HCPs) offering this service even to patients without access to traditional health care settings.
In addition to AI for DR screening gaining traction, prescreening with the same retinal image can also be assessed via other AI algorithms to detect CVD, CKD, and more. Unlike traditional screening, which is performed on indicated populations and often requires the patient’s proactive request in the testing process, prescreening can be conducted at a population level with patient consent. The use of retinal images may provide patients with the possibility for health checks while enabling HCPs to leverage existing health care interactions and data to identify individuals who may require further evaluation in primary care or by a specialist.
Such prescreening initiatives may benefit a diverse range of individuals, particularly those at risk who are unaware of their health risks and those who do not proactively visit a physician. This approach may be especially advantageous for people who lack access to health care facilities due to comorbidities or transportation limitations. Additionally, it may benefit individuals in underserved areas by expanding access to affordable screening and also early detection for serious health conditions, especially in regions with lower median household incomes, higher poverty rates, or fewer high school graduates. Such individuals tend to have fewer ECPs per 10,000 Medicare beneficiaries and fewer eye examinations performed per 100 Medicare beneficiaries. Furthermore, as of January 2025, there were 1,116 primary care health professional shortage areas, with 892 located in rural areas, affecting an estimated 76.3 million people.
For HCPs and payers, prescreening may provide considerable advantages in terms of augmenting evidence-based clinical practices, quality improvement, and efficiency. It may lead to a transformative shift in chronic disease screening and longitudinal monitoring, including diagnosing diseases at early stages, enabling proactive clinical risk stratification, and personalizing disease prevention strategies as well as therapeutic management.
Implementation of Healthcare From the Eye Into Established Workflows
Technology such as AI and imaging may further advance efforts to drive preventative care to improve health outcomes. Elevating the ability to screen for ocular and systemic diseases by implementing prescreening into existing health care workflows requires development of protocols that seamlessly integrate technologies for retinal imaging and AI assessment of the images.
In primary care clinics, effective prescreening for systemic conditions may offer benefits. To potentially minimize disruption to existing workflows, retinal imaging could be added to the initial patient assessment along with collection of traditional vital signs. AI assessment of the images occurs automatically, and findings are available to the doctor while the patient is still in the examination room at the point of care. If Healthcare From the Eye prescreening can be implemented at the appropriate sensitivity and specificity levels, the findings may complement other examination findings and even suggest the need for additional testing that would not routinely be performed. In some cases, prescreening might indicate the need for a referral to a specialist for further evaluation. For example, prescreening for CKD through retinal imaging can detect microvascular changes associated with kidney impairment, promoting additional kidney function tests. This integration may ensure prompt identification of potentially serious conditions, and having the information while the patient is still in the office facilitates timely referrals.
In ECP settings, retinal imaging often is performed as part of an eye examination. However, challenges arise when there is not a subsequent pathway for specialized management to other HCPs, if needed. To address this, establishing effective communication channels and partnership agreements between ECPs and other HCPs or health care networks seems essential to ensure that patients receive necessary follow-up care.
In decentralized health care settings, including home-based settings, medical assistants or nurses can perform prescreening, which may be particularly beneficial to individuals with limited mobility or transportation challenges. The results of the retinal prescreening examination should be visible to the patient’s doctor within minutes, therefore, any needed referrals or additional care can be obtained.
Integrating such prescreening approaches into electronic health record (EHR) systems would seem to be essential for optimizing workflow and data management. For example, advancements in EHR integration can simplify the review and follow-up of retinal images for screening and presumably should have a positive impact on workflow efficiency. Additionally, ensuring data interoperability across EHR systems would seem to be essential for reducing redundant prescreenings and screenings by streamlining patient data sharing. In turn, this boosts efficiency and coordination among HCPs. Cloud-based clinical data and workflow platforms likely will play a key role in securely implementing AI-powered solutions while maintaining established workflows. Furthermore, integrating prescreening into EHR systems will be vital for tracking health outcomes. They allow ECPs, PCPs, and patients to comprehensively monitor health outcomes. For instance, connecting PCPs with ECPs for patients living with diabetes should enable simultaneous monitoring and evaluation of both diabetes and DR, potentially leading to more efficient utilization of health care resources and better therapeutic outcomes. The ophthalmology community is developing AI inference capabilities with Fast Healthcare Interoperability Resources standards to streamline clinical workflows, potentially ensuring that information seamlessly integrates back into the EHR for enhanced patient care and data management.
In brief, facilitating prescreening in a coordinated care system among ECPs, PCPs, and other health care stakeholders may be essential. A triage system to identify patients needing further testing and ensuring these patients are not lost to follow-up also would seem to be important as it enhances efficient resource allocation and patient management. Moreover, fostering commonalities and interconnectedness among health care systems might optimize patient care delivery and outcomes.
Driving Adoption Through Sustainable Models
In one proposed reimbursement structure for prescreenings, HCPs would be compensated for each individual service they deliver, including prescreening procedures. Under this system, payments are made based on standard Current Procedural Terminology codes assigned to specific services. This structure ensures that HCPs receive direct payment for capture of retinal images and each prescreening procedure performed, aligning financial incentives with the provision of services. Additionally, specialists who conduct initial visits for referred patients will receive reimbursement for their specialized care and treatment. This framework has already been shown to be successful in DR screening programs.
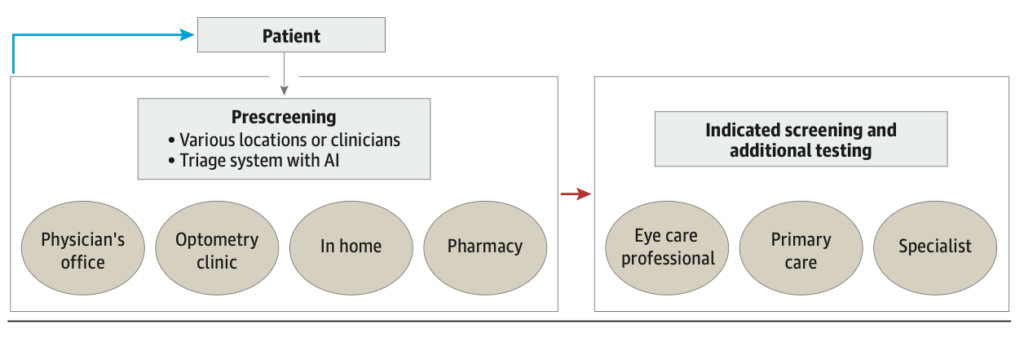
Prescreening for conditions from the eye is aligned with value-based care. The Centers for Medicare and Medicaid Services created the Part C & D Star Ratings to provide quality and performance information to Medicare beneficiaries to assist them in choosing their health and drug services. The Star Ratings include measures applying to 5 broad categories: (1) outcomes, (2) intermediate outcomes, (3) patient experience, (4) access, and (5) process.
Multiple ongoing pilot projects are evaluating how the previously mentioned prescreening ecosystem can scale and remain financially sustainable. These programs will investigate various financial models, alternative payment models, and value-based care innovation programs for the newer algorithms that do not have established reimbursement codes.
Engaging with stakeholders, such as pharmaceutical companies, HCPs, and government agencies, might provide a foundation for developing effective mechanisms that foster innovation to facilitate implementation of such prescreening initiatives. These efforts should also focus on advocating for equitable access to prescreening opportunities, adhering to clinical guidelines, and offering financial returns for payers, thus making health care more inclusive and affordable. The multidisciplinary approach also may create an opportunity to evaluate the financial impact on health care systems. Documenting that prescreenings in a coordinated care system reduce health care costs through earlier intervention and optimized resource utilization (including fewer specialist visits), may be crucial. Exploring potential reimbursement models and incentives for these screenings adds complexity, as stakeholders navigate health care financing nuances to find sustainable solutions. The program may not be effectively implemented until there is government support for Healthcare From the Eye prescreening services, especially for uninsured and low-income populations.
Potential Obstacles and a Look Into the Future
Overcoming potential obstacles for integration of prescreening within a coordinated care system likely requires a multifaceted strategy. In addition to regulatory and financial challenges, ethical and safety concerns may hinder the widespread adoption of AI solutions in clinical settings.
To optimize the impact of prescreening, more FDA-cleared AI systems are needed. Obtaining FDA clearance for sophisticated medical-grade AI technologies may be costly and time-consuming, presumably to ensure benefits are balanced with safety; this may delay the deployment of innovative solutions into clinical practice. The distinction between FDA clearance pathways such as the 510(k)-clearance process vs the de novo classification affects the speed at which prescreening solutions can be introduced to the market. Faster approval processes may accelerate the availability of innovative solutions.
Another area is the development of improved technology for such prescreening applications in homecare and other decentralized settings such as retail stores or pharmacies. Ideally, these devices should be portable, durable, and easy to use while offering the same high levels of accuracy and reliability as devices used in clinical settings.
Data privacy and security are also crucial concerns. As stewards of patients’ health care data, health care organizations should ensure that patient data are protected and properly managed. This means that each organization should prioritize cybersecurity and invest in the infrastructure that supports the protection of health care data. Moreover, federated learning may help by enabling data to reside within the control of the health care organization. An alternative model, the so-called opt-in/out model allows patients to have choice about whether their data are included.
Additionally, patients, HCPs, and health care organizations are not the only stakeholders. AI developers must be confident that the intellectual property of their algorithms is not exposed during the process of AI testing. Newer technology-based approaches to ensuring privacy, such as confidential computing, may help provide both data stewards and AI developers with the confidence that neither patient data nor the AI algorithms will be exposed during the AI development, validation, or testing process.
Furthermore, it may be important to assess whether current health care systems can handle the increased patient volumes that advanced AI-powered retinal imaging prescreening technologies may bring early on in a patient’s clinical journey. On the one hand, the infrastructure for general screening or early disease detection ideally should be scalable enough to manage more patients without sacrificing the quality of care. On the other hand, the shift toward early clinical management of chronic conditions may lead to better prognosis over time, with potentially remarkable medical and socioeconomical benefits in multiple levels: better quality of life for individual patients, optimization of health care resources with less severe diseases, and overall benefit for society at large by addressing the main causes of morbidity and mortality globally. Although promising, implementation of such a program presumably requires trustworthy technologies with both high sensitivity and specificity for the targeted diseases. A truly personalized health care system ideally should be accessible and affordable for high-risk patients, while reducing the overall clinical burden for low-risk patients for sustained feasibility. However, prescreening everyone may not always be cost-effective and may burden certain health care systems. Moreover, prescreening which is cost-effective and valuable in some health care systems may not be cost-effective or valuable in other health care systems.
The required performance of such technologies also includes rigorous testing of AI systems on local datasets to assess their performance across diverse populations and identify potential biases because patient safety is paramount. AI systems that are not sufficiently accurate or are biased risk creating distrust among the already overwhelmed HCP communities, potentially leading to lack of or even resistance to adoption.
One should also focus on the challenge of providing follow-up care for at-risk patients who lack access to health care or insurance. Innovative strategies are needed to ensure underserved populations receive continuous care regardless of their socioeconomic status or insurance situation. One way to potentially overcome this obstacle is to ensure that widespread deployment of prescreening solutions by ECPs, PCPs, pharmacies, malls, retail offices, and home visits are digitally connected through various image and data management platforms.
The adoption of prescreening technologies also may be influenced by payment models and reimbursement processes. By pushing for policy reforms, obtaining sufficient funding, and gaining government support, systemic barriers can be overcome and advancements in preventive health care delivery may be achieved.
Collaboration among stakeholders—HCPs, technology developers, and policymakers—is potentially essential for innovation, the development of new solutions needed for effective integration of Healthcare From the Eye prescreening into routine clinical practice, and to enable AI to be applied in a trustworthy and responsible manner. Organizations such as the Coalition for Health AI (CHAI) and the Trustworthy & Responsible AI Network (TRAIN) may help define important responsible AI principles and determine how best to operationalize those principles.
It seems vital to nurture a culture of iterative learning and ongoing improvement in preventive care. By embracing this mindset of constant refinement and adaptation, stakeholders presumably can keep up with emerging developments in health care to optimize patient outcomes.
Recommendations
Clinical researchers, HCPs/ECPs, health care organizations, pharmaceutical companies, and other key users:
A. Health economic analysis is essential for successful implementation. The relevant data should be collected and impactful measures should be developed to demonstrate return on investment, improve patient outcomes, and enhance HCP experience and training to drive meaningful policy changes.
B. Conduct more research on the delivery of oculomics, and explore conditions beyond DR, CVD, CKD, Alzheimer disease or dementia, multiple sclerosis, and other diseases.
C. Gain more experience in optimizing workflows for integrating and implementing prescreening in a coordinated care system.
Retinal imaging device manufacturers, AI developers, and implementers (picture archiving and communication system [PACS], EHR, and other software platform organizations):
A. Deliver robust, yet easily implementable, methodologies for mitigating privacy risks and security concerns associated with clinical data utilization.
B. Test AI solutions on heterogeneous datasets to ensure responsible AI practices.
C. Improve the interoperability of data within EHR systems, particularly for eye-related data. This will minimize redundant prescreenings and facilitate seamless patient data sharing.
Policymakers:
A. Support approaches that increase access to affordable health care and address health equity. Government programs should encourage and fund efforts to integrate Healthcare From the Eye prescreening.
B. Identify innovative funding mechanisms and reimbursement models to address scalability, adoption, and sustainability challenges for such prescreening initiatives.
Conclusions
Healthcare From the Eye with prescreening provides a potentially transformative opportunity for preventive health care. This approach has the potential to enhance early disease detection, improve access to care, and reduce costs. By leveraging existing infrastructure and fostering collaboration among stakeholders, a more equitable and effective health care system may be achieved.



